Adult Distal Radius Fractures
(also known as a "broken wrist")
Distal radius fractures are some of the most common fractures (the medical term for "broken
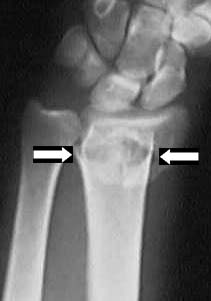
This is an xray of a distal radius fracture.
The arrows indicate the location of the
fracture. Note that the color of the bone
(the radius) is not uniform, with areas of
increased white and increased black. This
is, in part, how Dr. Nelson knows where
the fracture is. The small bones of the
wrist are seen at the top of the xray, there
is no fracture here. The black spaces between
the bones are the joints.
bone"). There are almost 600,000 distal radius fractures per year in the United States, so you are not alone. You might also hear this called a Colles' Fracture, after Abraham Colles, who described it, but this term is not used by current researchers in the field. The radius is the forearm bone on the thumb side (in the xray above, it is the one on the right). Distal radius fractures are generally caused by a fall on an outstretched hand. The fracture is almost always within an inch of the wrist joint, and may extend into the joint. The radius above is fractured at this location: about one inch from the wrist joint.
Fracture types can be described as "extra-articular" (which means the fracture line does not extend into the joint) or "intra-articular" (which means the fracture line does extend into the joint; this is the more serious type of fracture). They can also be described as "comminuted" (which means the bone is broken into several or many small pieces) or not comminuted. The most serious type of fracture is the comminuted, intra-articular fracture.
The second bone of the forearm is called the ulna. In the xray above, the ulna is on the left side of the image. The very tip of the ulna is called the ulnar styloid. It is commonly fractured (broken) when the distal radius is fractured. It itself rarely needs treatment. There is a fibrocartilaginous structure called the triangular fibrocartilage complex (a real mouthful, eh?), or abbreviated as the TFC, or TFCC. This structure stabilized the joint formed at the wrist by the radius and the ulna, called the distal radioulnar joint, or DRUJ. The stability of the DRUJ needs to be evaluated in each distal radius fracture. Sometimes this is fixed by fixing the ulnar styloid, but most often it is fixed by fixing the TFC.
Treatment
The treatment options are quite varied, depending on the exact nature of your fracture, your age, and your activity level. The treatment options include a cast, internal fixation with a plate, percutaneous pin fixation, external fixation, or a combination of these modalities. It is an area of very vigorous research and Dr. Nelson has been actively involved in distal radius research since 1990 (the external fixator below was designed by him in 1992). The treatments, both surgical and non-surgical, have changed greatly in the last few years. There are so many new ways to treat this fracture that it is difficult for most surgeons to keep up with all the new developments in this area. Here are some examples of the kinds of treatment that are available.
Internal Fixation Plate
 |
This is an example of an internal fixation plate. Almost all distal radius fractures that need surgery will get this treatment. The actual plate is on the right, and an xray of the plate on a patient is on the left. |  |
External fixation
 |
 |
|
Treatment of Distal Radius Fractures
The treatment decision is very complex. As noted above, the factors that are important are the exact nature of your fracture, your age, and your activity level. The nature of the fracture relates to the current alignment of your bones (what position they are in) and whether or not that alignment is acceptable. If it is acceptable, then you will probably get a cast. If it is not acceptable, Dr. Nelson needs to reduce the fracture (put the bones in a better position). Sometimes the fracture is of the sort that can be pushed into place without surgery (called a "closed reduction"), and sometimes the fracture needs surgery to push the bones into place (called an "open reduction", because the skin needs to be "opened" for surgery). Usually, if the broken bones need surgery (in medical terms, the fracture needs open reduction), some kind of metal implant will be needed to hold the bones in the proper place while they heal. Most of the time, the metal implant (often called a "plate", but it does not look like a dinner plate! See the photo at the top, above, for an example of a plate) needs to be placed on the bones.
As you can see, the treatment decision is very complex. At Dr. Nelson's course, the International Distal Radius Fracture Course, three whole days are spent on this topic! Dr. Nelson will explain it to you in the office. Hopefully, this page will help you to understand.
What Can I expect While It Is Healing?
This is a great and simple question, but the answer is not simple. It depends on many factors: the nature of your fracture, its treatment, your response to treatment, your age, and your activity level, among many other factors. But it is an important question, and needs to be answered. Whether you have surgery or just a cast, most patients do not need narcotic pain medication, just prescription-strength, non-narcotic medication. All patients are given a prescription for narcotic medication, but about 80% of them decide that the non-narcotic medications work so well that they choose not to take the narcotic. Dr. Nelson is a member of the International Association for the Study of Pain and has presented his post-operative pain management results at the international meeting. His pain managment regimen has been proven to work for over 18 years: about 80% of patients never take any narcotic medication. You can read about his pain management regimen here. If patients take narcotic medication, is it usually for only a few (less than 5) days.
While the bone is healing, we will be taking xrays. The purpose of the xray is NOT to check the degree of healing, which is what most patients think. It is to check the position of the bone while it is healing. This seems surprising to many patients, so let me explain. The xray is a great test, but it has its limits. The xray is great for checking bone, because a bone has a lot of calcium in it, and the calcium is what shows up in the xray. The new bone that is forming has little or no calcium in it, and it does not show up at all on xray. It only shows up after it gets calcified, which is about a month after it is formed, but this degree of calcification is slight. Your fracture may be completely healed but only show up slightly on the xray. However, the xray is very good at examining the alignment of the bones, so I know that when it finally heals, it will be in the correct alignment.
If you have a cast, it is usually on for six weeks, then hand therapy is started. If you have internal fixation, you get a splint for three days and then hand therapy starts to get your wrist joint moving. No splint is usually needed three days after surgery. Casts must be kept dry (use a plastic bag while showering), and surgical incisions need to be kept dry only for five days. No matter what kind treatment you get, you should be actively exercising your fingers, elbow, and shoulder, so they don't get stiff. Dr. Nelson will decide, based on your exact fracture, when you can start strengthening exercises; until then, just work on motion.
Many patients want to know if the metal plate in their arm will set off the airport security alarms. No, it will not. The plate is made of titanium, which is not magnetic. Dr. Nelson has carried two of the plates through security in his pocket as a test and the alarms did not go off! No patient has reported that their plate set off the detectors. In any case, the Transportation Security Administration has instructed patients who set off the alarm (usually total hip or total knee patients) to merely show the agent your scar (for the arm or knee) or ask for a pat-down (for the hip). They will verify that the plate set off the alarm by using the wand over your incision. It will not be a problem.
What Can I Expect After It Has Healed?
Almost all patients have their surgery as an out-patient, which means that you come in, have surgery, and leave the hospital about two hours after surgery. Most patients get a soft dressing plus a small splint. The splint should be removed in 3 days. Most patients are referred to hand therapy, which starts at three days. If you have a therapy appointment, you can let the therapist remove the splint and dressing. The dressing is discontinued five days after surgery and you can leave it open or, if you prefer, cover it with a bandaid. I like the NexCare brand of waterproof bandaids; get the "knee and elbow" size. You can get the incision wet when you shower or take a bath after this time (five days after surgery). Most patients will be seen in the office at 10 days.
Everyone wants to know, "Can I return to all my former activities?" This is a great and simple question, but without a simple answer. Everyone has some stiffness in their wrist after treatment (remember, you fell on your hand hard enough to break the bone, so the joint and all the soft tissues around it are mad at you!). This is why almost everyone is referred to hand therapy at three days after surgery, to start moving the soft tissues and help them to become flexible.
Everyone wants to know, "How much will it hurt?" Most patients will need to take some pain medication for a few days (see above), and some may need it for 10 or so days. Few patients need any pain medication other than aspirin, Tylenol, or Motrin after 10 days. Almost everyone will have some discomfort in their wrist as it heals over a period of three to six months. If you do not develop arthritis, you will not have pain after this. You will still experience some minor discomfort for a year or so.
Almost everyone ends up with some stiffness that is permanent; how much depends on your injury, your age, if you already have some stiffness and arthritis, and how hard you work in hand therapy. The forearm motion that is usually the stiffest is turning your palm up (called "supination), in the position as if you were trying to hold some water in your cupped hand. There is also some limitation in flexion and extention, which are the motions bending your hand toward your palm or toward the back side of your hand. However, almost all patients get about 80% of their range of motion back and most get more than 90%. Almost everyone can return to almost all their activities. The exception would be any activity that takes an extreme of motion, such as the Yoga pose "downward dogs", which requires 90 degrees of wrist extension. But this is a rather radical activity: few people find that they are unable to do their former activities.
Most patients return to normal recreation and work activities, and most do not have permanent pain. The most limiting fracture type is a comminuted, intra-articular fracture, and these patients will have the greatest amount of stiffness, may have pain, and are at risk for developing arthritis. Extra-articular fractures usually do not develop arthritis.
The amount of stiffness is largely what determines what activities you can return to. Most patients who are active playing non-contact and non-impact sports such as bike riding, swimming, etc., can return to those activites soon after the fracture. Non impact activities such as swimming can be resumed at a week or so. Minor stress activities like riding a bike can be resumed at about 4-6 weeks. Most patients who are active playing contact sports or sports that involve impact, such as tennis, golf, baseball, football, etc, can return to those activites, starting at about 4 months. Most patients who do heavy labor, such as carpentry, plumbing, etc, can return to work at 2 months with restrictions, and regular work without restrictions at 4 months. Most patients who do lighter labor such as painting, or office work activities such as handwriting, keyboards, telephone, etc, can return to work at 1 to 2 months. I do not allow people to do activities where they are at risk for falling for about four months. These are only general guidelines so you have some idea of what to expect, and your specific restrictions will be determined by your individual circumstances.
Dr. Nelson has a particular interest in distal radius fractures. He has chaired several international courses exclusively on distal radius fractures, and has lectured on them in the United States, England, France, and Italy. He has invented one of the external fixators that are used to treat these fractures (shown above) and one of the internal fixation plates (shown above). These devices are sold throughout the world. He is actively involved with anatomy research, developing newer methods of distal radius fracture treatment and with teaching surgeons from around the world about how to treat distal radius fractures. He is the Webmaster of a site, eRadius, devoted exclusively to distal radius fractures. (eRadius is designed to teach experienced orthopedic and trauma surgeons; it is not designed for patients.)
If you want to read another page I have written about distal radius fractures, click here.
If you want to read what patients have written about their own experiences after a distal radius fracture,click this for patients who had a cast for the distal radius fracture and click this for patients who have had surgery for a distal radius fracture.
If you want to learn more about fractures in general, see Fractures in General.
Some of my research on the anatomy of the distal radius is here. (This is intended and written for surgeons, not patients, but it might be interesting anyway.)
There is some interesting data developing on Vitamin C, RSD, and distal radius fracture here.
